Coronary Artery Disease
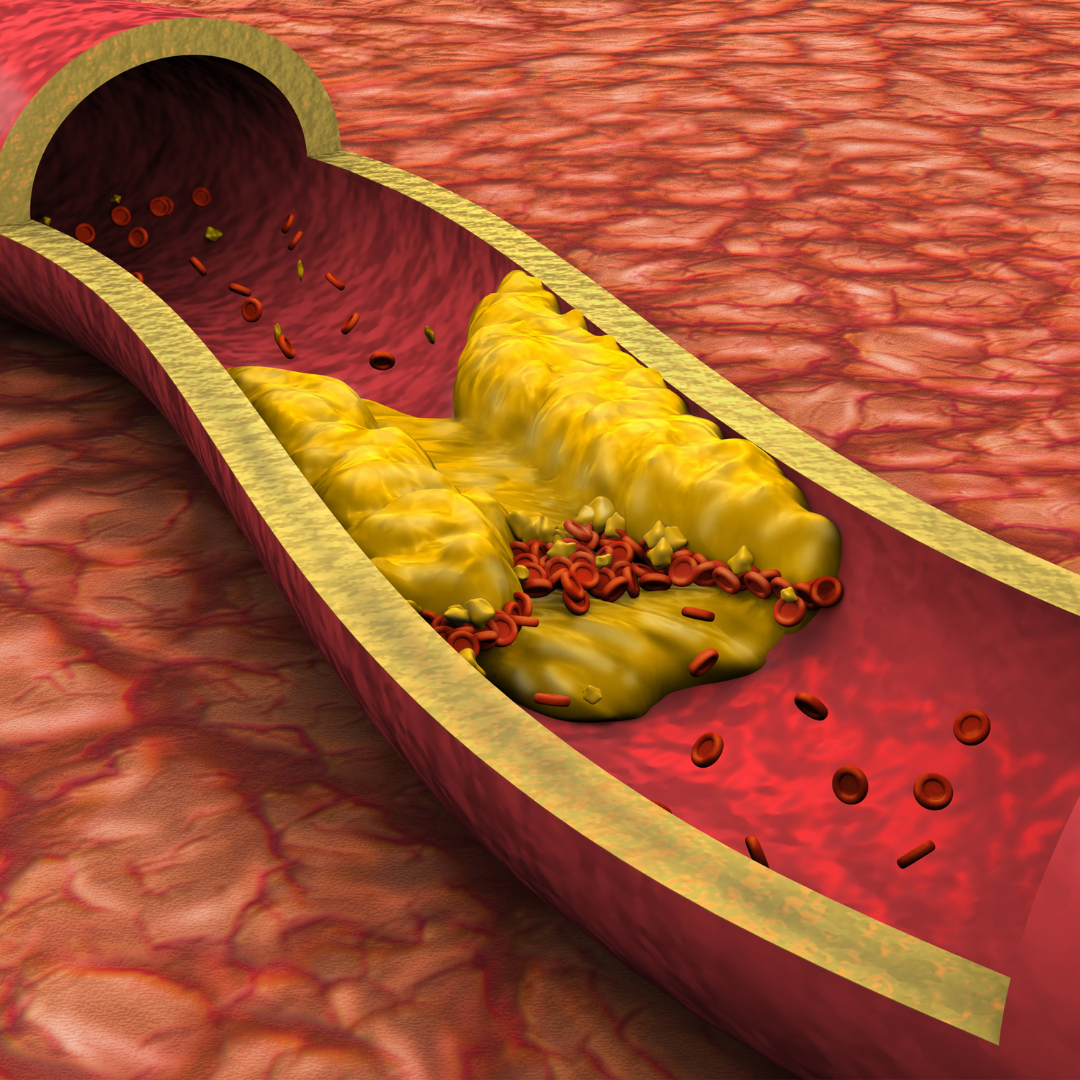
Coronary artery disease develops when fatty deposits gradually accumulate within the arteries that supply blood to the heart muscle.
Over time, these deposits may restrict blood flow, particularly during exertion. In some cases, a plaque can rupture unexpectedly, causing a heart attack.
Although common, coronary artery disease is highly treatable — particularly when managed early by a specialist with advanced expertise in coronary intervention.
Symptoms may include:
Chest pressure or tightness
Breathlessness on exertion
Reduced exercise tolerance
Fatigue out of proportion to activity
Subtle or atypical symptoms (particularly in women)
During your clinic visit, assessment is unhurried and comprehensive. Your symptoms will be explored in addition to your lifestyle, risk profile, family history and long-term cardiovascular goals.
Why Does It Happen?
Coronary disease develops when traditional cardiovascular risk factors damage the artery lining over time.
The most important risk factors include:
High blood pressure – puts strain on artery walls
High cholesterol – contributes to plaque formation
Diabetes – accelerates artery damage
Smoking – significantly increases clot and plaque risk
Family history of early heart disease
Sedentary lifestyle and excess weight
Stress and poor sleep
For women, symptoms may be more subtle and risk is sometimes under-recognised.
How Is Coronary Artery Disease Diagnosed?
Diagnosis depends on your symptoms and overall risk profile.
Investigations may include:
ECG
Blood tests
Echocardiogram
CT coronary angiography
Stress testing
In some cases, invasive coronary angiography
The goal is not just to “find a blockage,” but to understand whether the narrowing is significant, whether it is causing symptoms and whether treatment will improve outcomes.
How Is It Treated?
Treatment depends on severity and symptoms.
Lifestyle optimisation
Often the most powerful intervention includes structured exercise, a Mediterranean-style diet, weight optimisation, smoking cessation and stress management
Medication
Cholesterol-lowering therapy (statins and other agents), antiplatelet therapy, blood pressure control and/or anti-anginal medications
Coronary intervention
(See section on coronary angiography and angioplasty below for more details)
In selected patients, a narrowed artery can be treated with a stent to restore blood flow. This is performed via a small tube inserted through the wrist or groin and usually requires an overnight stay.
Intervention is recommended when:
Symptoms persist despite medication
There is high-risk anatomy
There is evidence of threatened heart muscle
Can Coronary Disease Be Reversed?
Plaque can be stabilised and sometimes partially regressed with intensive cholesterol lowering, strict risk factor control and sustained lifestyle change. The most important goal is preventing plaque rupture, which causes heart attacks.
Coronary Angiography
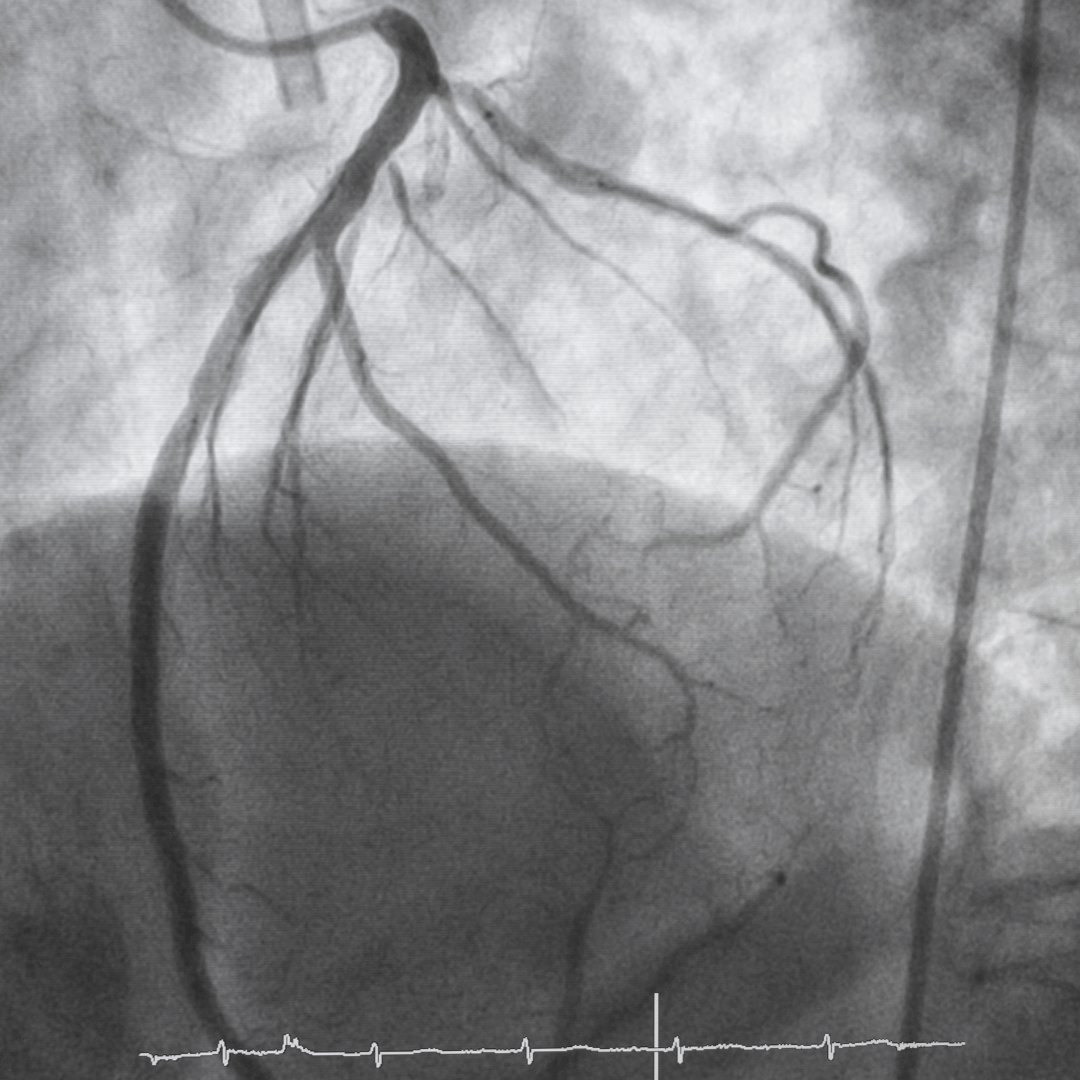
Coronary angiography is the most accurate way of assessing the coronary arteries.
It is a minimally invasive procedure performed in a specialist cardiac catheter laboratory. A very fine tube (catheter) is inserted, most commonly through the wrist (radial artery), and guided to the heart under X-ray guidance.
Contrast dye is injected to allow us to see:
Whether arteries are narrowed or blocked
How severe the narrowing is
Which part of the heart is affected
Whether intervention would improve symptoms or prognosis
The procedure typically takes 20–40 minutes and is performed under local anaesthetic. Most patients go home the same day.
Is It Safe?
Coronary angiography is very safe when performed by experienced operators. Serious complications are uncommon. You remain awake throughout and can speak to the team at all times.
Safe practice includes:
Radial (wrist) access whenever possible
Careful patient selection
Clear explanation before and after the procedure
Coronary Stenting (Angioplasty)
— Restoring Blood Flow to the Heart
If a significant narrowing is identified, it can often be treated immediately with angioplasty and stent implantation.
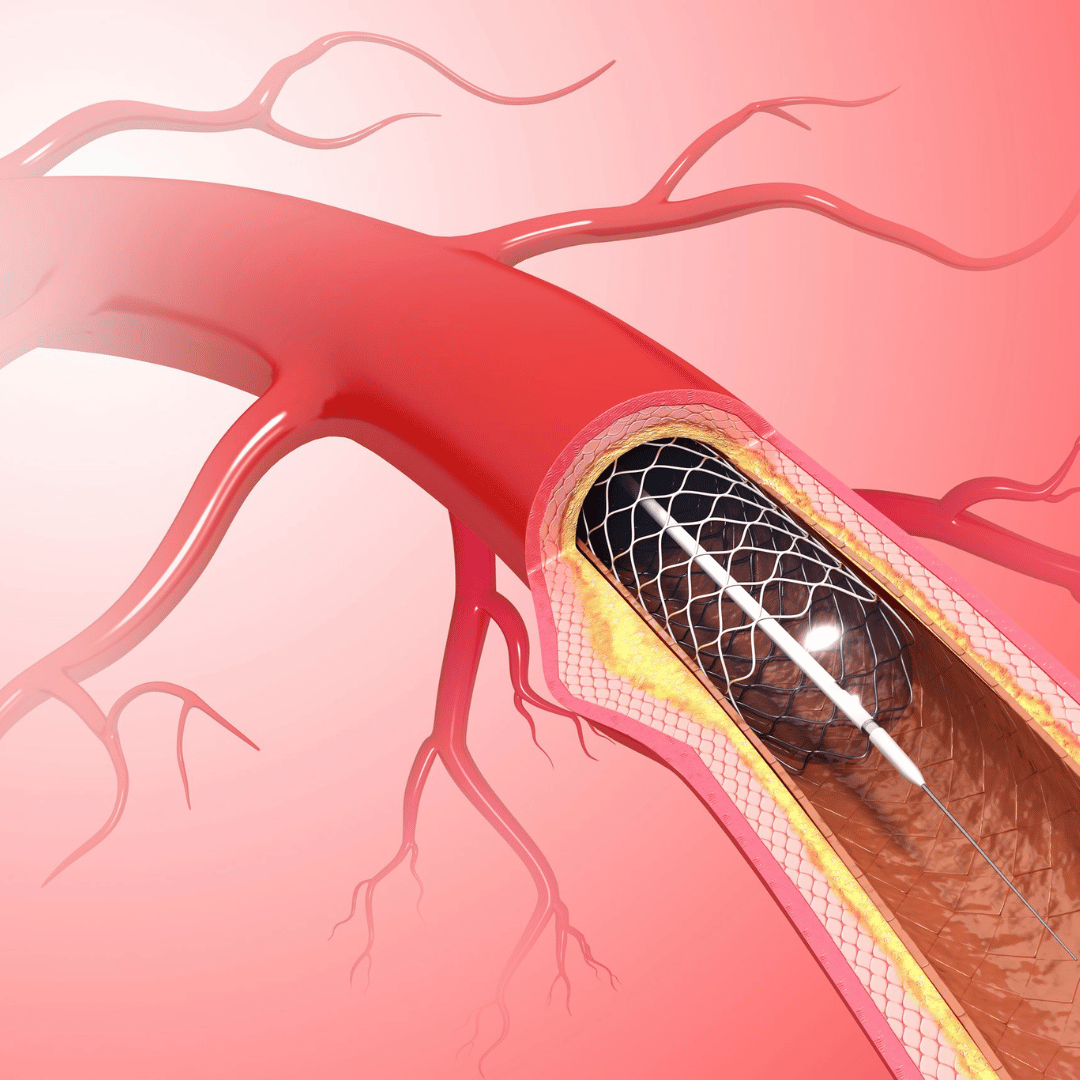
A stent is a tiny metal scaffold inserted into the narrowed artery. It opens the blockage restores blood flow, relieves angina symptoms and reduces risk in certain high-risk blockages. Modern stents are drug-eluting, meaning they slowly release medication to reduce re-narrowing.
How Is a Stent Inserted?
1. A small balloon is positioned across the narrowing
2. The balloon is gently inflated to open the artery
3. The stent is deployed and remains permanently in place
4. Blood flow is immediately improved
The procedure is usually completed through the wrist and most patients stay one night.
Do All Narrowings Need a Stent?
No, one of the most important aspects of modern cardiology is ensuring that we only treat blockages that are truly significant.
In many cases, we use advanced techniques during angiography, including:
Pressure wire assessment (to measure blood flow limitation)
Intravascular imaging such as IVUS or OCT
Physiological assessment to confirm whether a narrowing is causing ischaemia
This ensures treatment is necessary, evidence-based and tailored to you. Avoiding unnecessary stents is just as important as performing them expertly when required.
What Are the Benefits of Stenting?
For patients with angina:
Rapid symptom relief
Improved exercise capacity
Better quality of life
For patients with acute coronary syndromes (heart attack or unstable angina):
Restoration of blood flow
Reduction in heart muscle damage
Improved survival
What Happens After a Stent?
After the procedure you will take antiplatelet medication to prevent clotting. Most patients resume normal activity within a few days. Cardiac rehabilitation may be recommended and ongoing risk factor optimisation remains essential.
A stent treats a specific narrowing, it does not cure coronary artery disease, which is why prevention remains crucial.